Home > Clinical depts > Department of Breast Surgery
Department of Breast Surgery
Tatsuya Onishi, Chisako Yamauchi, Tsuguo Iwatani, Rurina Watanuki, Yuki Eguchi, Kayono Onishi
Introduction
We treat patients with operable malignant mammary glands. Our main professional practices are diagnosing breast disease, providing surgical treatment and conducting follow-up for breast cancer patients. The Department of Breast Surgery is committed to providing the latest, most comprehensive breast treatments for our patients. The multidisciplinary approach to the diagnosis and treatment of cancer is performed with the cooperation of related specialists.
Our department focuses on “minimally invasive surgery” and performs thorough investigations for oncologically safe approaches, with lower morbidity and good cosmesis. For example, although sentinel lymph node (SLN) biopsy has been established as the standard care for clinical node negative patients, omitting axillary lymph node dissection (ALND) for positive SLNs has been included in clinical practice as an expanded indication. Preoperative systemic therapy provides the opportunity for a curative operation or breast-conserving surgery to avoid mastectomy. Moreover, we can provide breast reconstructive surgery in collaboration with the Department of Plastic and Reconstructive Surgery. These procedures will contribute to a better quality of life for patients with breast cancer.
The team and what we do
For the regular activities of our department, a daily morning round is scheduled for inpatients by all staff. Moreover, our weekly preoperative diagnostic imaging conference is conducted to discuss each patient's surgical treatment planning. A clinical conference to decide on the treatment courses by multidisciplinary breast care team members is held twice a month. A monthly pathological conference on breast cancer is also conducted. At these conferences, individual cases are presented to a team of highly trained cancer specialists, including radiologists, breast surgeons, pathologists, radiation oncologists, and medical oncologists. Our multidisciplinary team approach to breast cancer treatment provides superior-quality care to patients.
Changes in the annual number of patients with breast cancer who underwent surgery are shown in Table 1. Surgeries were performed on 476 patients with primary breast cancer and 66 patients with recurrent or iatrogenic breast cancer.
Table 1. Number of primary breast cancer patients who underwent surgery during 2017-2021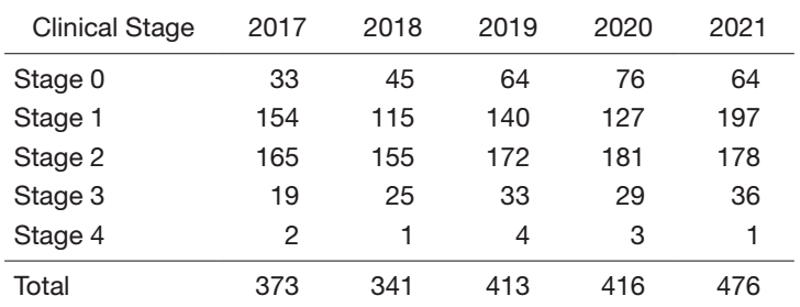
Hospital East
Thirteen immediate breast reconstruction surgeries were included. Of the patients with primary breast cancer, 95 (20%) underwent primary systemic therapy. The types and number of operative procedures performed in 2021 are shown in Table 2. The rate of breast-conserving surgery was 47% (224/476). Sentinel node biopsy was performed on 380 patients, and 370 patients were spared from ALND. The number of immediate breast reconstruction surgeries using tissue expanders decreased in 2019 because the tissue expanders were recalled due to breast implant-associated anaplastic large cell lymphoma; however, there was a recovery in the number of surgeries in 2021, continuing from 2020 (2019: 5 cases; 2020: 13 cases).
Table 2. Types and number of procedures performed in 2020 for primary breast cancer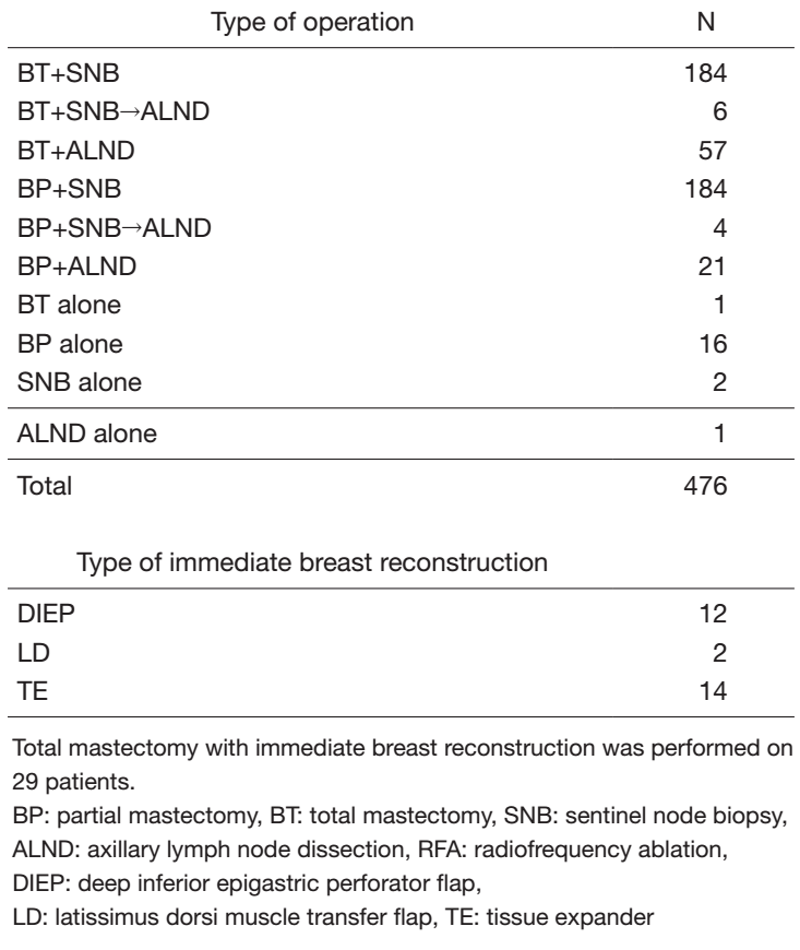
Research activities
We contribute to establishing new standard treatments for breast cancer patients by actively enrolling participants in clinical trials. The clinical trials we are currently conducting are as follows.
Clinical trials
1) Single-arm confirmatory trial of endocrine therapy alone for estrogen receptor-positive, low-risk ductal carcinoma of the breast in situ (JCO1505, LORETTA Trial): This is a single-arm interventional study to confirm whether endocrine therapy alone for ER-positive low-risk DCIS is safe and effective compared with the current standard treatment.
2) Study for avoiding mastectomy using trastuzumab, pertuzumab and radiation for breast cancer (JCOG1806, AMATERAS-BC): This is a single-arm study to confirm the efficacy of avoiding surgical treatment for HER2-positive breast cancer patients who received neoadjuvant chemotherapy and achieved complete response.
3) Radiofrequency ablation (RFA) using a Cool-tip electrode system: A phase II study of RFA without resection was performed for T=<1.5 cm, N0 breast cancer patients using a Cool-tip electrode system (RAFAELO study); patients were offered RFA therapy for early breast cancer (PO-RAFAELO study).
4) Effectiveness of primary tumor resection for metastatic breast cancer (JCOG 1017): In this clinical trial, a primary tumor resection plus systemic therapy arm is compared with a systemic therapy alone arm in metastatic breast cancer.
5) Intensive vs. standard post-operative surveillance in high-risk breast cancer patients (JCOG1204, INSPIRE Trial): This is a randomized phase III trial to confirm the superiority of intensive follow-up to standard follow-up in terms of overall survival in high-risk breast cancer patients.
6) A prospective observational study to explore the impact of risk-reducing mastectomy and surveillance on mental and psychological status and quality of life in patients with hereditary breast cancer or ovarian cancer
7) Investigation on the performance inconsistency of deep learning models for mammogram classification in different populations: An international, multi-center study.
Education
Our goal is to train residents to become leaders in breast cancer treatment from clinical and research perspectives. On the clinical side, we improve the understanding of breast diseases through various conferences and provide surgical guidance. We also provide guidance for conference presentations and writing papers, along with support for obtaining medical specialties and degrees.
Future prospects
We will deliver appropriate postoperative follow-up care, which has been a long-term concern in breast cancer medical care. We also aim to further develop surgical approaches with minimally invasive and cosmetic surgery. Moreover, we will construct a treatment system that is conscious of fertility preservation, hereditary cancers and appearance with an awareness of the patients' viewpoint.
List of papers publishe
Journal
1. Onishi T, Mihara K, Matsuda S, Sakamoto S, Kuwahata A, Sekino M, Kusakabe M, Handa H, Kitagawa Y. Application of Magnetic Nanoparticles for Rapid Detection and In Situ Diagnosis in Clinical Oncology. Cancers, 14:2022
2. Iwatani T, Inoue E, Tsugawa K. Validation of the predictive accuracy of health-state utility values based on the Lloyd model for metastatic or recurrent breast cancer in Japan. BMJ open, 11:e046273, 2021
3. Iwatani T, Noto S, Tsugawa K. Changes in Health State Utility Values in Japanese Patients with End-Stage Breast Cancer. Current oncology (Toronto, Ont.), 28:4203-4212, 2021
Book
1. Watanuki R, Nagayama A, Hayashida T, Kitagawa Y. Chemoprevention for Breast Cancer. In: Nakamura S, Aoki D, Miki Y (eds), Hereditary Breast and Ovarian Cancer Molecular Mechanism and Clinical Practice, Singapore, Springer, pp 129-148, 2021
